By Valerie Carsey
More and more surgeons are recommending lymphatic drainage after surgery. Can you heal without it? Absolutely. However, many people find that post-surgical manual lymphatic drainage speeds up the healing process and makes recovery more comfortable.
Manual lymphatic drainage is a gentle, superficial technique focused on moving excess fluid in your tissues toward your body’s primary drainage sites — the neck, armpits, and groin. After surgery, these fluids need to be carefully routed around scar sites. If you are dealing with lymphedema specifically, I recommend working with a lymphedema specialist, either in addition to or instead of working with me, as they have additional training in lymphedema, wound care and compression garment fitting.
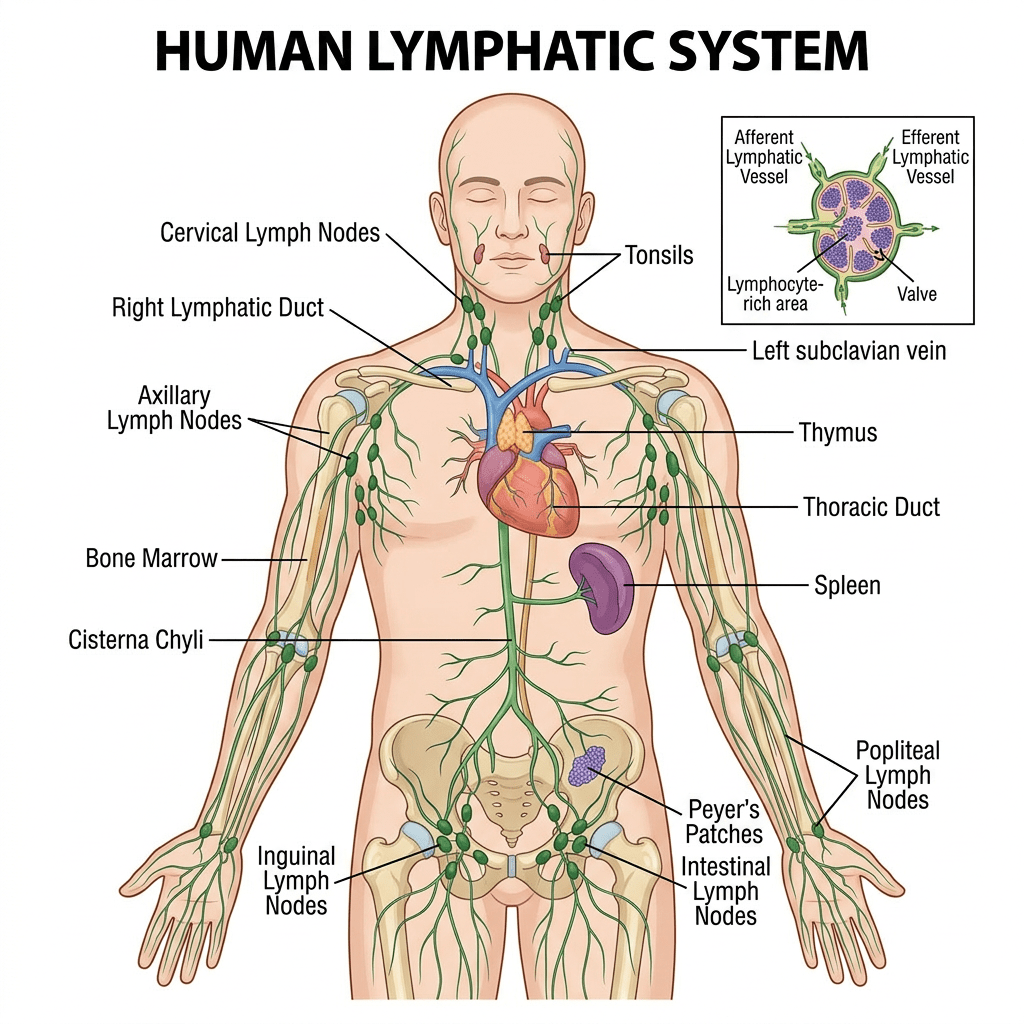
What Is the Lymphatic System and What Does It Do?
The lymphatic system is part of your circulatory system. While the blood system (veins and arteries) is a closed loop starting and ending at the heart, the lymphatic system is an open network of vessels throughout the body. It picks up fluid and substances that cannot be drained or reabsorbed by the blood system.
Benefits of Manual Lymphatic Drainage Include:
· Transporting immune cells that help fight infection
· Stimulating lymph vessel activity and fluid movement
· Improving reabsorption and promoting drainage of accumulated fluid
· Removing waste products from the body
· Reducing the tendency toward tissue fibrosis (scar tissue formation)
· Providing an analgesic effect and promoting relaxation
· Redirecting lymph flow around surgical sites
· Helping prevent post-surgical lymphedema
Training
I believe it important to find someone properly trained in post-surgical lymphatic drainage — either a lymphedema specialist or a manual lymphatic drainage practitioner with advanced post-surgical training.
I am a certified manual lymphatic drainage practitioner with advanced training in Oncology and Post-Surgical Manual Lymphatic Drainage through ACOLS (the Academy of Lymphatic Studies), as well as Neurolymphatic Drainage training through Monarch Continuing Education.
Internationally recognized training programs (per LANA — the Lymphology Association of North America) include: Academy of Lymphatic Studies, American Academy of Lymphatic and Wound Management, Brennan School of Innovative Lymphatic Studies, Chikly Health Institute, Dr. Vodder International, ILWTI, Klose Training, Lincoln Lymphedema, LymphEd LLC, Monarch Continuing Education, Norton School of Lymphatic Therapy, E-HIS Clinician Courses Ltd, O.ED.E.M.A. Academy, and the University of Wisconsin.
Recommended Schedule
Some schools teach that lymphatic drainage can begin as soon as 2–3 days after surgery; others recommend waiting a full week. I prefer to wait until the incisions have closed, which typically takes about a week.
After that initial week, and with your surgical team’s approval, I recommend the following schedule:
· Twice a week for three weeks
· Once a week for two weeks
· Re-assess at the 6-week mark
t the six-week mark most surgeons conduct a follow-up visit. With their approval, this may be the earliest that scar work can begin. That said, individual needs vary, and you may be advised to come in more or less frequently. To help manage costs, I offer discounted session bundles in 5- and 10-pack packages.
When to Hold Off on Post-Surgical Lymphatic Drainage
Always keep your surgical team informed and follow their guidance. If they advise against lymphatic drainage, defer to their recommendations.
In addition, certain post-surgical symptoms are a signal to pause treatment and contact your surgical team:
· The area is red and hardened
· Swelling is disproportionate in one area versus other regions of your body (example, one breast is much larger than the other)
· You have a fever
· Your incision has reopened
· You have signs of infection
In Closing
Research increasingly supports the use of manual lymphatic drainage after surgery — whether that is a cosmetic procedure, cancer tumor removal, or orthopedic surgery like a knee replacement. With benefits ranging from relaxation to a reduced risk of lymphedema, it can be a valuable addition to your post-operative care.
References
· NIH (October 22, 2024). “Brain Waste-Clearance System Shown in People for First Time.” https://www.nih.gov/news-events/nih-research-matters/brain-waste-clearance-system-shown-people-first-time
· Archives of Physical Medicine and Rehabilitation, Vol. 94, Issue 11, pp. 2103–2111 (November 2013). “Randomized Trial Investigating the Efficacy of Manual Lymphatic Drainage to Improve Early Outcome After Total Knee Arthroplasty.” https://www.sciencedirect.com/science/article/abs/pii/S0003999313004619
· Zimmermann, A. et al. Lymphology 45, 103–112 (2012). “Efficacy of Manual Lymphatic Drainage in Preventing Secondary Lymphedema After Breast Cancer Surgery.” https://formationdrainage.ch/wp-content/uploads/2025/09/efficacite-du-dlm-preventif-apres-ca-sein.pdf
· Masson, I.F.B. et al. Indian Journal of Plastic Surgery 47(01): 70–76 (2014). “Manual Lymphatic Drainage and Therapeutic Ultrasound in Liposuction and Lipoabdominoplasty Post-Operative Period.” https://www.thieme-connect.com/products/ejournals/abstract/10.4103/0970-0358.129627
Edited by AI